Allergic rhinitis, commonly called hay fever, is often dismissed as a minor condition. However, for many veterans, chronic nasal inflammation, breathing problems, fatigue, and sleep disruption can significantly affect daily functioning and employability. Recognizing this impact, the Department of Veterans Affairs offers compensation through the VA disability rating for allergic rhinitis when the condition is service-connected.
This detailed guide explains the rhinitis VA rating criteria, how the PACT Act changed eligibility requirements, and what veterans can do to strengthen a claim.
Table of Contents
Understanding Allergic Rhinitis as a VA Disability
Allergic rhinitis is an immune response that occurs when the body reacts to airborne allergens such as pollen, dust mites, mold, or pet dander, triggering inflammation in the nasal passages and causing persistent symptoms. It is one type of rhinitis, a broader group of conditions that also includes non-allergic (vasomotor) and atrophic rhinitis. For veterans, environmental exposure during deployments, particularly smoke, dust, airborne toxins, and chemicals, can increase the risk of developing chronic rhinitis.
Common symptoms of allergic rhinitis include:
- Sneezing and coughing
- Runny or congested nose
- Itchy or watery eyes
- Postnasal drip
- Sinus pressure or headaches
- Fatigue and difficulty sleeping
Veterans may develop several forms of rhinitis, but two types are most relevant in VA claims:
Seasonal Allergic Rhinitis: Triggered by outdoor allergens such as pollen or grasses, typically worse during spring, summer, or early fall.
Perennial Allergic Rhinitis: Occurs year-round and is triggered by indoor allergens like dust mites, cockroach residue, mold, or pet dander.
Both forms may qualify for a VA allergic rhinitis rating if symptoms become chronic or significantly interfere with daily functioning. Chronic rhinitis is generally defined as symptoms lasting longer than three months or recurring frequently over time.
While allergic rhinitis is rarely life-threatening, its long-term effects can interfere with work, sleep, concentration, and mental health, which is why the VA considers it a compensable condition.
How Military Service Can Lead to Allergic Rhinitis
Many veterans face a higher risk of developing respiratory conditions due to hazardous exposures encountered during military service.
Common risk factors of allergic rhinitis include:
- Burn pit smoke and airborne particulate matter
- Sandstorms and desert dust
- Mold and poor air quality in barracks
- Chemical fumes and industrial solvents
- Smoke and environmental pollutants
Burn Pit Exposure and Rhinitis Claims
One of the most widely recognized causes of rhinitis is exposure to burn pits, which released toxic smoke from burning plastics, fuel, medical waste, ammunition, and other materials. Smoke and particulate matter from these sites in Iraq, Afghanistan, and other regions could travel long distances, exposing service members to harmful airborne pollutants. Veterans who served in Southwest Asia or post-9/11 deployment zones also faced poor air quality and often reported higher rates of respiratory problems.
Because of these service exposures, many veterans pursue a VA claim for the condition after discharge. Although nonallergic rhinitis also exists, VA compensation is most often granted for allergic or chronic rhinitis linked to environmental exposure.
How the VA Rates Allergic Rhinitis (Diagnostic Code 6522)
The VA rates allergic rhinitis under Diagnostic Code 6522 (38 CFR § 4.97) based on the degree of nasal obstruction and the presence of nasal polyps.
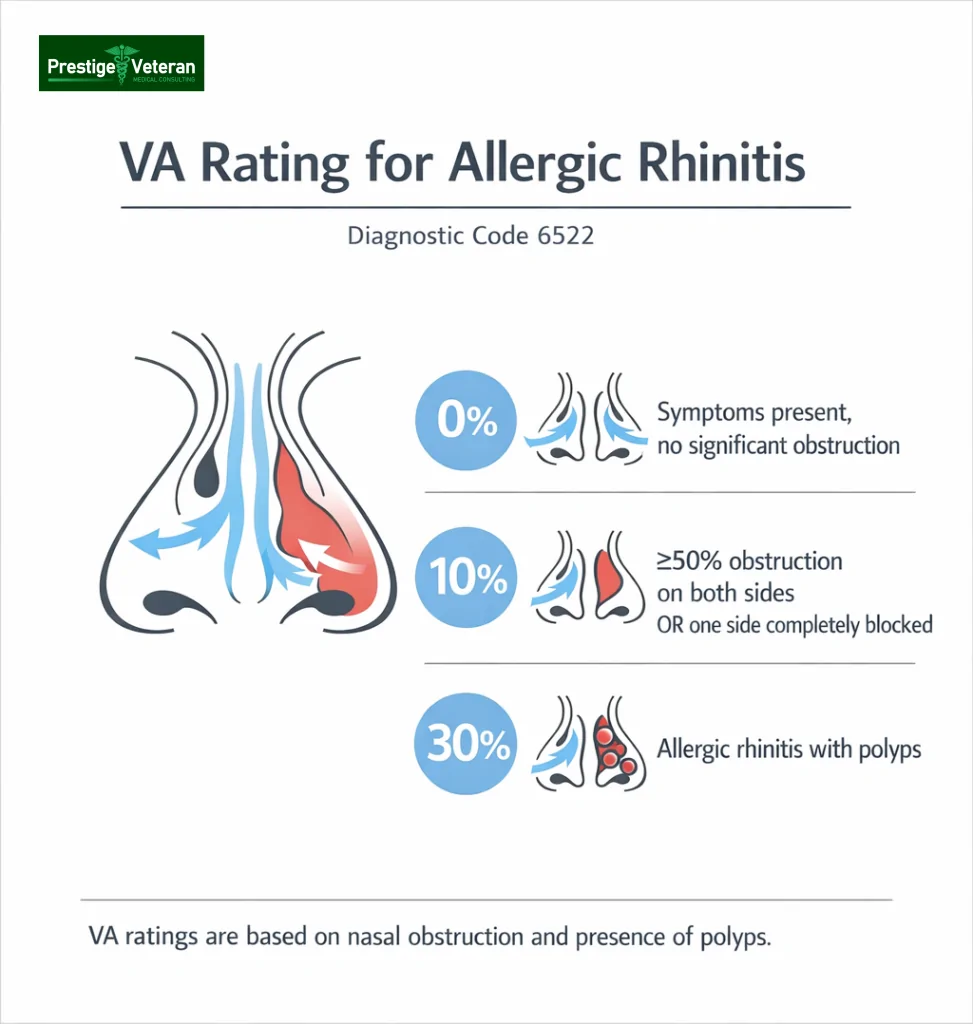
VA Rating Criteria (DC 6522 – Allergic or Vasomotor Rhinitis):
- 30% rating: Presence of nasal polyps.
- 10% rating: No polyps, but greater than 50% obstruction of nasal passages on both sides or complete obstruction on one side.
- 0% rating: Symptoms are present and are recognized as service-connected, yet do not meet the compensable criteria. At this level, you can still seek treatment through VA healthcare and pursue increased ratings if symptoms worsen.
Rating for allergic rhinitis mainly depends on objective findings from an ENT exam (or VA C&P exam), such as documented polyps and the examiner’s assessment of nasal obstruction.
Example: A veteran with ongoing nasal congestion and breathing difficulty undergoes a VA exam that shows complete blockage in the right nasal passage but no polyps, resulting in a 10% disability rating under DC 6522.
The maximum schedular rating for allergic rhinitis is 30%; however, you may receive higher total compensation through combined ratings, secondary service connection, or TDIU when disabilities prevent your ability to work.
The PACT Act and Presumptive Service Connection for Rhinitis
The Honoring Our PACT Act of 2022 significantly expanded presumptive service connection for veterans with respiratory conditions, including chronic rhinitis. Previously, veterans were often required to submit detailed medical evidence to prove a direct connection between their illness and military service. Under the PACT Act, the Department of Veterans Affairs now acknowledges the long-term health effects of exposure to particulate matter, burn pits, and other airborne hazards, reducing the burden of proof for veterans.
Qualifying Locations and Service Areas
Rhinitis may be presumed service-connected if it develops within ten years of qualifying military service in designated regions, for instance:
- Southwest Asia theater of operations beginning August 2, 1990
- Afghanistan, Syria, Uzbekistan, and Djibouti from September 19, 2001, onward
- Iraq, Kuwait, Bahrain, Qatar, Saudi Arabia, and the United Arab Emirates
- Somalia and other recognized areas including Egypt, Jordan, Lebanon, Syria, and Djibouti
With the PACT Act, chronic rhinitis, along with asthma and sinusitis, was added to a new burn-pit–related presumptive list, effective August 10, 2022, expanding access to health care and disability compensation for affected veterans.
Department of Veterans Affairs, Presumptive Service Connection for Respiratory Conditions Due to Exposure to Particulate Matter, 86 Fed. Reg. 42724 (Aug. 5, 2021).
What This Means for Veterans
Under the VA presumptive rules, veterans who served in qualifying locations no longer need to prove a direct medical nexus between service and their condition. Meaning, they can qualify for an allergic rhinitis VA rating by showing:
- A current diagnosis
- Qualifying service in eligible locations
- Honorable discharge
Veterans previously denied may reopen the issue by filing a supplemental claim using VA Form 20-0995 and citing environmental exposure as the cause. Overall, the PACT Act has made benefits more accessible and the claims process simpler for veterans with rhinitis.
Ways to Establish Service Connection for Allergic Rhinitis
To receive VA disability compensation, veterans need to show that their allergic rhinitis is tied to their military service. The VA recognizes three main ways to establish this connection, and the right path often depends on a veteran’s service history, exposures, and medical records.
Direct Service Connection
To establish direct service connection for allergic rhinitis, veterans must meet three key requirements, as outlined in 38 CFR § 3.303:
- Current diagnosis: Medical evidence from a qualified healthcare provider confirming allergic or chronic rhinitis.
- In-service event, illness, or exposure: Records or credible evidence showing exposure to allergens, burn pit smoke, dust, chemicals, or other respiratory irritants during service.
- Medical nexus: A medical opinion linking the current condition to the in-service exposure or event.
In most cases, the VA will schedule a Compensation & Pension (C&P) exam to verify your diagnosis, evaluate symptoms, and provide a medical opinion that can affect your disability rating.
Secondary Service Connection
Secondary service connection may apply when allergic rhinitis is caused or worsened by another service-connected condition under 38 CFR § 3.310. For example, veterans with sinusitis, asthma, or other respiratory disorders may qualify if those conditions aggravate nasal inflammation.
Presumptive Service Connection
Presumptive service connection may be available under the PACT Act and VA rules in 38 CFR § 3.307 and § 3.309 for veterans exposed to burn pits or other toxic environments. In qualifying cases, the VA may presume chronic rhinitis is service-related, so a separate medical nexus may not be required.
In all cases, strong supporting evidence such as VA or private treatment records, deployment history, or lay statements can significantly improve the likelihood of approval.
How to File an Allergic Rhinitis VA Claim
Veterans seeking a disability rating can obtain application steps for self filling on the VA’s website or coordinate with an accredited legal professional.
Considerations for Your Disability Claim:
- Obtain a current diagnosis of allergic rhinitis from a qualified medical professional.
- Gather service records that show when nasal or sinus symptoms began during service, or exposure to irritants such as dust, smoke, or burn pits, if applicable.
- Provide medical records, including treatment history, nexus letters (for non-presumptive claims), or, if available, a DBQ completed by a private physician to strengthen your case.
- Submit VA Form 21-526EZ to apply for disability compensation (In accordance with VA’s instructions). Attach all supporting evidence and file it by one of these methods:
- Online through the VA benefits portal
- Mail to the VA Evidence Intake Center
- Submit in person at a VA regional office or with the assistance of a Veterans Service Officer (VSO) or another accredited legal professional.
- Attend the VA Compensation & Pension (C&P) exam, if scheduled, as the findings are used to evaluate your disability.
- Track your claim status online and respond promptly to any VA requests for any additional records. Be sure to keep copies of all submissions.
Carefully review your VA decision letter and consider an appeal if the disability rating seems too low or if service connection is denied.
How to Prepare for Your C&P Exam for Rhinitis
After you file a disability claim, the VA usually schedules the Compensation and Pension exam by phone or letter, and missing the appointment or failing to reschedule can lead to denial. The purpose of this exam is to assess the severity of the condition and confirm your eligibility for a VA disability rating for rhinitis.
Before the visit, confirm that your contact information is updated. Review your records, since the examiner will study your claims file, including service and medical history.
What Happens During the Exam?
A C&P exam for allergic rhinitis is typically conducted by a VA or contracted clinician who will take these steps:
- Initial clinical evaluation. The examiner will evaluate your symptoms, review prior treatments, and ask detailed questions about the onset of the condition, triggers, frequency, and how rhinitis symptoms affect daily life.
- Physical assessment. Expect a targeted physical inspection of the nasal passages, breathing, and related structures. In some cases, imaging or respiratory testing may be ordered.
- Discussion of functional impact. Be prepared to explain limitations such as sleep disturbance, difficulty concentrating, or interference with work, as these factors influence the disability rating. Be honest and detailed, for instance, you can say “The pressure in my sinuses gives me headaches that keep me awake at night.”
- Completion of the DBQ. The examiner records findings on a Disability Benefits Questionnaire (DBQ), noting the degree of nasal obstruction, polyps, hypertrophy of the turbinates, diagnostic results, and occupational impact.
Finally, VA reviewers consider the examiner’s findings and medical opinions to determine service connection and appropriate disability rating. Remember to obtain a copy of your C&P exam results for your personal records.
Tip: You may also support your claim by submitting additional evidence, such as DBQs completed by a private provider, supporting medical records, nexus opinions, and documentation of toxic exposures under PACT Act rules.
Download the VA Disability Benefits Questionnaire (DBQ) for Sinusitis/Rhinitis and Other Conditions
Secondary Conditions to Allergic Rhinitis: Get a Higher Combined Rating
Allergic rhinitis can lead to or worsen other medical conditions because persistent nasal inflammation, immune activation, and airway irritation affect multiple body systems. In VA disability claims, these secondary service connections may qualify you for additional compensation when supported by medical evidence.
Common secondary conditions to allergic rhinitis include:
- Chronic sinusitis – Persistent nasal congestion and inflammation may block sinus drainage, allowing mucus buildup and bacterial growth, leading to recurrent or chronic sinus infections.
- Bronchial asthma – Allergic inflammation in the upper airway may extend to lower airways (“united airway” effect), increasing bronchial irritation and thereby worsening asthma symptoms.
- Obstructive sleep apnea – Ongoing nasal obstruction from allergic rhinitis can impair airflow during sleep, promote mouth breathing, and worsen airway collapse or sleep apnea.
- Nasal polyps – Long-term inflammation of the nasal lining can cause benign growths (polyps), which further obstruct airflow and worsen congestion.
- Eustachian tube dysfunction: Allergic swelling in the nasal cavity may block the Eustachian tube opening, causing pressure imbalance, ear fullness, or poor drainage.
- Chronic otitis media: Persistent Eustachian tube dysfunction can allow fluid to collect in the middle ear, increasing the risk of recurrent, chronic ear infections.
- Allergic conjunctivitis: Allergens that trigger nasal inflammation may also irritate the eye conjunctiva, leading to redness, itching, burning, and excessive tearing.
- Gastroesophageal reflux disease (GERD): Chronic throat clearing, coughing, and altered breathing patterns can aggravate gastroesophageal reflux disease by increasing pressure and irritating the esophagus.
- Chronic laryngitis (chronic throat irritation): Continuous post-nasal drainage and inflammation may irritate the throat and larynx, causing hoarseness, frequent throat clearing, and persistent throat discomfort.
- Migraine headaches: Chronic nasal inflammation, sinus pressure, and sleep disturbance related to allergic rhinitis can trigger migraines or increase frequency and severity.
- Mental health disorders: Symptoms such as poor sleep, fatigue, breathing difficulty, and poor quality of life may contribute to depression or anxiety disorders.
For example, a veteran whose chronic nasal congestion contributes to sleep apnea could receive a separate disability rating for that condition. Filing a secondary claim is an important strategy to receive a higher combined disability percentage and increase your overall compensation.
When claiming secondary service connection, a nexus letter from a qualified healthcare professional explaining that a secondary condition is “at least as likely as not” caused or aggravated by allergic rhinitis is usually critical.
100% TDIU for Allergic Rhinitis: When Symptoms Prevent Employability
Total Disability based on Individual Unemployability (TDIU) allows veterans with service-connected conditions, such as allergic rhinitis, to receive compensation at the 100% rate when they are unable to maintain substantially gainful employment.
Although allergic rhinitis has a maximum VA rating of 30% under DC 6522, TDIU may still be awarded when the condition is severe or when it is combined with other service-connected conditions such as asthma, chronic sinusitis, sleep apnea, or depression.
Schedular TDIU Criteria
Under 38 CFR § 4.16(a), you may qualify for TDIU on a schedular basis if either of the following conditions is met:
- One service-connected disability rated at 60% or higher, or
- Two or more service-connected disabilities with:
- A combined disability rating of 70% or higher, and
- At least one disability rated at 40% or higher.
Extraschedular TDIU Criteria
If percentage requirements are not met but service-connected conditions still prevent employment, veterans may be considered for extraschedular TDIU under 38 CFR §4.16(b). In some cases, separate extraschedular ratings under 38 CFR §3.321(b)(1) may apply if allergic rhinitis causes unusual or severe symptoms not fully covered by VA rating criteria.
Example: A veteran exposed to burn pits who develops allergic rhinitis and asthma may experience severe fatigue, sleep disturbance, and breathing difficulty, making regular work in dusty or fume-filled environments impossible. In such cases, qualifying for TDIU benefits can provide necessary financial support when employment is no longer sustainable.
The VA website instructs that you can file VA Form 21-8940 to apply for TDIU and may submit employer information using VA Form 21-4192. Additionally, evidence such as medical records, employment history, and physician nexus opinion, or lay statements describing work limitations, may be helpful for building a strong TDIU claim.
Tips to Support a VA Disability Claim for Rhinitis
Many VA claims are denied due to insufficient evidence or unclear service connection. Veterans can improve approval chances and support a higher rating by:
1. Keep a Symptom Journal That Shows Daily Impact
Instead of simply noting that allergies occur, record how they interfere with life. Track specific symptoms like nasal congestion, sneezing, coughing fits, headaches, fatigue, and sleep problems. Note how often flare-ups occur, what triggers them, and how long they last. For example, noting that exposure to smoke fumes at work frequently forces you to leave due to coughing or nasal irritation provides concrete evidence of occupational impact.
2. Follow Prescribed Treatment Plans Consistently
Using medications such as antihistamines, nasal sprays, or immunotherapy indicates that your rhinitis requires ongoing management. Keep a consistent record of prescriptions and refills, as the VA often looks for evidence that symptoms persist despite treatment.
3. Document Worsening Symptoms for a Higher Rating
Regularly inform your healthcare provider if symptoms worsen, such as increased breathing difficulties, frequent sinus infections, or sleep disturbance, so progression is recorded in your medical history. Ensure updated evaluations, imaging, or a private Disability Benefits Questionnaire (DBQ) note measurable findings like nasal polyps or increased nasal obstruction. This objective evidence supports a higher VA rating for rhinitis.
4. Ask for a Strong Medical Nexus Letter
When service connection is required, ask your physician to write a detailed medical opinion clearly explaining how environmental exposures or service conditions can trigger chronic inflammation in the nasal passages. Make sure the nexus letter references your service history, symptom progression, and the medical reasoning showing the condition is “at least as likely as not” (50/50 probability) related to service.
Submitting an independent medical opinion can be helpful for non-presumptive claims where symptoms must establish a direct or secondary link to military service.
5. Submit Buddy Statements or Lay Evidence
Statements from family members, coworkers, or fellow service members can help confirm the real-life impact of your respiratory illness. For instance, a coworker might describe how often you use nasal sprays during a shift or how fatigue affects your productivity. Family members can note sleep disturbances, frequent coughing, or irritability caused by chronic symptoms.
Witnesses can submit VA Form 21-10210 (Lay/Witness Statement) to provide written firsthand accounts in support of your claim.
6. Document Environmental and Service-Related Exposure
Gather service records, deployment orders, or duty location histories that show exposure to airborne hazards such as sandstorms, particulate matter, industrial pollutants, or burn pits. Show your participation in the Airborne Hazards and Open Burn Pit Registry, as it helps document reported exposures and related health concerns in an official VA record.
Even brief exposure to pollutants or poor air quality has been linked to chronic rhinitis, and documenting this exposure can support service connection and influence your VA rating.
Combining medical evidence, personal records, and exposure history helps present an honest picture of your condition, improving the chances of approval and a fair VA disability rating.
If Your Claim Is Denied: Review and Appeal Options
If the VA denies your disability claim, you still have options to continue pursuing benefits. Each option serves a different purpose, depending on whether you want a new review, to submit evidence, or to appeal to a judge.
If a claim is denied, VA’s Appeals Modernization Act notes that veterans can pursue:
- Higher-Level Review
A senior VA reviewer re-examines your claim using the same evidence. This is helpful if you believe the VA made an error in interpreting records or applying regulations. - Supplemental Claim
This option allows you to submit new and relevant evidence, such as updated medical records, imaging, or a stronger nexus letter, which may improve your chances of approval. - Board Appeal
You may appeal to the Board of Veterans’ Appeals, where a Veterans Law Judge reviews your case, with options to submit evidence or request a hearing.
Get official forms and step-by-step guidance at the VA Decision Review page.
Consider seeking help from a Veterans Service Officer (VSO), claims agent, or VA-accredited attorney who can help prepare the necessary evidence and support you throughout the appeals process.
Conclusion
Securing a fair VA rating for allergic rhinitis often requires patience, solid documentation, and a clear explanation of how the condition affects your daily life and ability to work. Staying organized, keeping medical records up to date, and following prescribed treatment can strengthen your claim as it progresses. Veterans who were exposed to burn pits, dust, or other airborne hazards should also consider whether presumptive service connection may apply, as this can simplify the process.
If the steps or evidence feel confusing, seeking guidance from an accredited representative or qualified professional can help you pursue the benefits and healthcare support you deserve.
Frequently Asked Questions (FAQs)
What do I say at a C&P exam for rhinitis?
At a C&P exam for rhinitis, clearly describe your symptoms, their onset and frequency, triggers, treatments, and how they affect your sleep, daily activities, and ability to work.
What is a 10% rating for allergic rhinitis?
A 10% VA rating for allergic rhinitis is assigned when there are no nasal polyps but there is greater than 50% obstruction of both nasal passages or complete obstruction on one side.
What is the VA disability percentage for rhinitis?
The VA rates allergic or vasomotor rhinitis at 0%, 10%, or 30% under Diagnostic Code 6522, depending on nasal obstruction and the presence of polyps.
How to prove my rhinitis to the VA?
You typically prove rhinitis to the VA by providing:
- Current medical diagnosis
- Evidence of in-service exposure or a qualifying presumptive service history, and
- Medical nexus or supporting documentation linking the condition to service.
Is rhinitis with polyps considered a VA disability?
Yes, rhinitis with nasal polyps is considered a compensable VA disability and generally qualifies for a 30% rating when service connection is established.
Also Read: Obstructive Sleep Apnea and Allergic Rhinitis in Veterans Disability
At Prestige Veteran Medical Consulting, a veteran-owned company, we specialize in Independent Medical Opinions (IMOs) known as Nexus letters.
Our purpose is to empower YOU, the veteran, to take charge of your medical evidence and provide you with valuable educational tools and research to guide you on your journey.
Understanding the unique challenges veterans face, our commitment lies in delivering exceptional service and support.
Leveraging an extensive network of licensed independent medical professionals, all well-versed in the medical professional aspects of the VA claims process, we review the necessary medical evidence to incorporate in our reports related to your VA Disability Claim.
Prestige Veteran Medical Consulting is not a law firm, accredited claims agent, or affiliated with the Veterans Administration or Veterans Services Organizations. However, we are happy to discuss your case with your accredited VA legal professional.