Back pain is a prevalent issue among veterans, often resulting from the physically demanding nature of military service. Recognizing the impact of spinal conditions, the Department of Veterans Affairs (VA) has established a detailed framework for evaluating and compensating veterans suffering from back-related disabilities. This guide delves into the intricacies of VA disability ratings for back pain, understanding the evaluation process, common secondary conditions, and steps that help maximize ratings.
Table of Contents
Common Back Conditions Recognized by the VA
The VA acknowledges various spinal conditions that can lead to chronic back pain. Some of the most commonly recognized service-connected back conditions include:
- Lumbosacral Strain (Diagnostic Code 5237): A condition characterized by muscle strain in the lower back, often resulting from overuse or injury.
- Degenerative Disc Disease (DDD) (Diagnostic Code 5242): The breakdown of intervertebral discs, leading to pain and reduced mobility.
- Spinal Stenosis (Diagnostic Code 5238): Narrowing of the spinal canal, which can compress nerves and cause pain or numbness.
- Spondylolisthesis (Diagnostic Code 5239): A condition where one vertebra slips over another, potentially causing instability and pain.
- Ankylosing Spondylitis (Diagnostic Code 5240): A form of arthritis that leads to inflammation of the spinal joints, potentially resulting in fusion of the vertebrae.
- Intervertebral Disc Syndrome (IVDS) (Diagnostic Code 5243): A condition involving herniated or bulging discs that can press on spinal nerves, causing pain and other symptoms.
Understanding the specific condition affecting your spine is crucial, as each has unique diagnostic criteria and implications for VA disability ratings.
VA’s Criteria for Back Pain Disability Ratings
The VA uses a standardized system to rate back pain and spinal injuries, based on how much they impair your ability to function, under 38 CFR § 4.71a – the General Rating Formula for Diseases and Injuries of the Spine.
The VA evaluates two main spinal regions:
- Thoracolumbar spine (mid and lower back)
- Cervical spine (neck)
The rating depends largely on Range of Motion (ROM), which must be measured using a tool called a goniometer during your Compensation and Pension (C&P) exam. The less you can bend, twist, or move without pain, the higher VA rating you may be assigned.
Thoracolumbar VA Ratings
- 10% Rating: Awarded when forward flexion measures between 60 and 85 degrees, or when minor symptoms like guarding, tenderness, or muscle spasms are present without causing abnormal gait or spinal alignment issues.
- 20% Rating: Granted when forward flexion falls between 30 and 60 degrees, or when the total spinal motion (combined range of motion) does not exceed 120 degrees. This also includes cases with muscle spasms or posture abnormalities like scoliosis or kyphosis caused by guarding.
- 40% Rating: Given when the forward bending ability is severely limited to 30 degrees or less, or when the entire thoracolumbar spine is stiffened (ankylosed) in a position considered functionally neutral or “favorable.”
- 50% Rating: Reserved for conditions where the thoracolumbar spine is completely immobilized in a poor or “unfavorable” position, affecting function more significantly.
- 100% Rating: This rating reflects the most serious condition, when both the thoracic and cervical parts of the spine are fixed in an unfavorable position, severely impairing mobility and function across the entire spinal column.
It’s important to note that ankylosis refers to the abnormal stiffness of joints and loss of mobility, due to fusion of bones.
Cervical Spine (Neck) VA Ratings
- 10% Rating: Applicable when neck flexion exceeds 30 degrees but stays within 40 degrees, or when the total movement range of the cervical spine falls between 170 and 335 degrees. This rating also covers cases with minor symptoms like tenderness, guarding, or muscle spasms that do not alter spinal alignment or walking ability.
- 20% Rating: Assigned if forward neck movement is limited to between 15 and 30 degrees, or if total cervical motion is restricted to 170 degrees or less. This rating level also applies when muscular problems like spasms or guarding are serious enough to affect posture or gait.
- 30% Rating: This rating is warranted when neck flexion is extremely restricted, 15 degrees or less or when the entire cervical spine is stiffened (ankylosed) in a position that is considered favorable for function.
- 40% Rating: Granted when the cervical spine is completely fused in a non-functional or unfavorable position, significantly limiting mobility.
- 100% Rating: Reserved for total spine fixation, when both the neck and thoracolumbar regions are rigid due to unfavorable ankylosis, representing the most severe impairment level.
Understanding these rating criteria helps veterans advocate for fair compensation based on the severity of their spinal limitations.
Intervertebral Disc Syndrome (IVDS) and VA Ratings
Intervertebral Disc Syndrome (IVDS) is one of the most prevalent spinal conditions veterans face. If a Veteran does not meet the criteria for a cervical or thoracolumbar spine rating based on range of motion or ankylosis, they may still qualify for VA disability compensation under Intervertebral Disc Syndrome (IVDS).
IVDS is a condition in which discs between your vertebrae degenerate or herniate, which can press against nerves and cause pain, numbness, and sciatica. Unlike standard back conditions that are measured by range of motion, IVDS is rated based on incapacitating episodes.
The VA rates IVDS claims under Diagnostic Code 5243:
- 10% Rating: Incapacitating episodes at least 1 week within the past year.
- 20% Rating: Incapacitating episodes totaling at least 2 weeks but less than 4 weeks.
- 40% Rating: Incapacitating episodes at least 4 weeks but less than 6 weeks.
- 60% Rating: Incapacitating episodes totaling at least 6 or more weeks in the past 12 months.
An incapacitating episode is defined as a period of acute signs and symptoms that requires bed rest prescribed by a physician and treatment by a healthcare provider.
Without doctor-prescribed bed rest in your medical records, the VA won’t assign a rating under this code, even if you have missed weeks of work.
The Importance of Range of Motion (ROM) Measurements
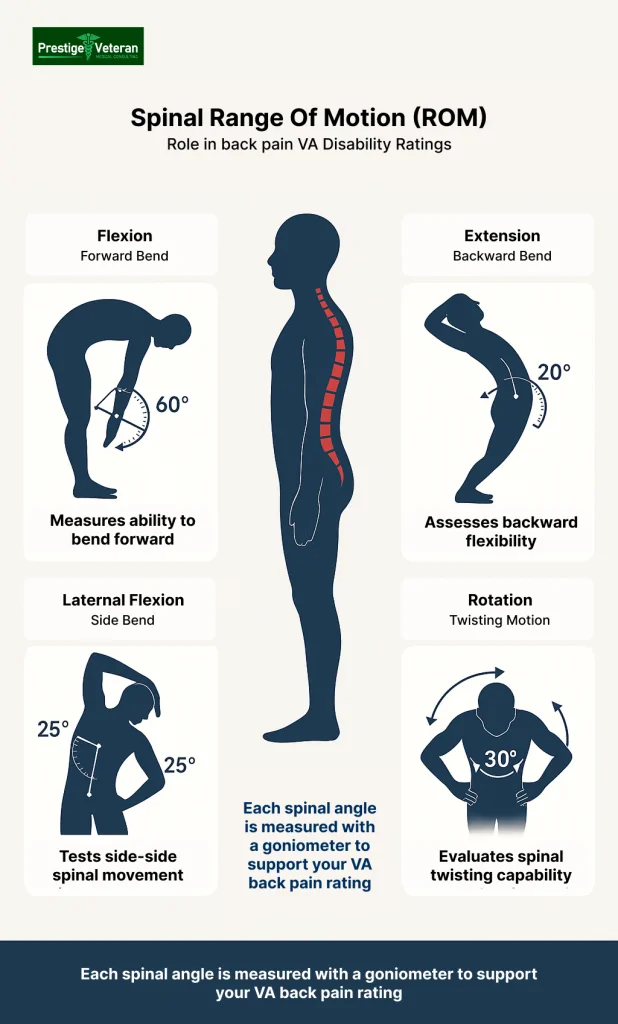
The precise assessment of spinal Range of Motion (ROM) is important for determining a fair and appropriate VA disability rating. During a Compensation and Pension (C&P) exam, a clinician will use a goniometer to measure the angles of spinal movement, including:
- Flexion: Bending forward
- Extension: Bending backward
- Lateral Flexion: Bending sideways
- Rotation: Twisting movements
These measurements provide objective data on a veteran’s functional impairment from back conditions, directly impacting the disability rating. Additionally, the range of motion test helps to strengthen medical evidence in a VA disability claim.
Functional Loss and the “Painful Motion” Principle
The VA recognizes that pain can significantly impact function, even if ROM measurements appear within normal limits. According to 38 CFR § 4.59, any evidence of pain during movement qualifies the condition for at least the minimum compensable disability rating. This is known as the “Painful Motion” principle. Therefore, if pain is noted during movement, a veteran should receive at least a 10% rating, acknowledging the functional loss due to pain.
Proving a Service Connection for Back Pain
To qualify for VA compensation for back pain, you must demonstrate a service connection by showing that your current back injury is directly related to your time in the military. Establishing this link involves submitting evidence for three components:
- A Current Diagnosis: You need a medical diagnosis for a back pain condition. Pain alone can qualify if it causes functional loss, thanks to the Saunders v. Wilkie ruling.
- An In-Service Event or Injury: This could include heavy lifting, combat trauma, repetitive strain from ruck marches, vehicle accidents, or impact injuries from airborne operations.
- A Medical Nexus: A nexus letter is an independent medical opinion linking your current diagnosis to your in-service event or injury. A well-supported letter from a provider familiar with VA claims can explain how your current back problems are “at least as likely as not” caused by your time in service. A nexus is always required; however, it does not have to come in the form of a formal letter. Your C&P examiner can provide you with a positive nexus at the exam if they believe there is enough information to support the connection.
Prestige Veteran offers expert Independent Medical Opinions written by qualified medical professionals to help veterans establish a clear link between their current back condition and military service.
Secondary Conditions Related to Back Pain
Back pain, particularly when service-connected, can trigger a range of secondary health issues that significantly impact a veteran’s quality of life and VA disability rating. Identifying and documenting these secondary conditions to back pain can qualify a veteran for additional VA disability compensation.
Common secondary conditions include:
1. Radiculopathy: Often stemming from spinal nerve compression, radiculopathy causes sharp, radiating pain, numbness, or weakness in the limbs. It’s a common secondary effect of spinal disc issues or herniation, especially in the lumbar or cervical spine.
2. Depression and Anxiety: Chronic pain can wear heavily on mental health. Veterans with ongoing back problems often develop depression or anxiety due to limitations on mobility, reduced independence, and lifestyle changes.
3. Sleep Disorders: Back pain often disrupts normal sleep patterns, potentially leading to insomnia or contributing to conditions like obstructive sleep apnea, especially when pain-related inactivity results in weight gain.
4. Joint Conditions (Knees, Hips, Ankles): Altered gait caused by back pain frequently places strain on surrounding joints, leading to secondary problems like osteoarthritis or chronic joint pain.
5. Gastrointestinal Issues: Long-term use of NSAIDs or pain medications for back pain can lead to GERD, ulcers, or gastritis. These are the conditions that diminish comfort and digestion.
6. Urinary Incontinence: In more severe spinal cases, nerve damage can impair bladder control, often pointing to conditions like cauda equina syndrome or spinal stenosis.
7. Erectile Dysfunction: Nerve damage affecting the lower spine can disrupt sexual function, leading to erectile dysfunction. It is also sometimes worsened by side effects from pain medications.
To prove a secondary claim, veterans must submit a nexus opinion indicating that the secondary condition is “at least as likely as not” caused or worsened by their primary service-connected back condition.
How to Get a 100% VA Disability Rating for Back Pain?
Getting a 100% rating for a back pain VA claim is uncommon, but it is possible if the condition leads to total disability and prevents the veteran from maintaining gainful employment. Here are some pathways:
Fixed or Unfavorable Spinal Position
To receive a 100% VA rating for back pain, a veteran must show that the entire spine, thoracolumbar and cervical, is immobile or stuck in an unfavorable alignment. If there’s any spinal movement or if it’s frozen in a neutral posture, the VA typically assigns a lower rating. Only complete, unfavorable fixation supports the highest possible disability percentage.
Total Disability Based on Individual Unemployability (TDIU) for Back Pain
Veterans suffering from service-connected back issues that hinder their ability to engage in substantially gainful employment might be eligible for Total Disability based on Individual Unemployability (TDIU). TDIU eligibility allows qualified veterans to receive compensation at the 100% disability rate, even if their total VA disability rating is under 100%.
You might qualify for TDIU compensation if:
- You have one service-connected disability rated at least 60% or higher, or
- You hold a combined VA disability rating of 70% or more, with at least one condition rated at 40% or higher.
- You are unable to maintain substantially gainful employment due to your service-connected disabilities.
Proving a TDIU claim may require strong documentation such as independent medical opinions, employment history, and vocational expert statements.
Temporary Total Ratings Due to Hospitalization
Veterans hospitalized for more than 21 days because of back pain may qualify for a temporary 100% VA disability rating. This benefit must be requested directly, as the VA won’t assign it automatically. The full rating may continue through the hospital stay and potentially beyond, depending on the post-discharge evaluation of the back condition’s severity.
What Happens in a Back Pain C&P Exam?
A Compensation and Pension (C&P) exam is one of the most influential steps in your VA disability claim for back pain. Conducted by a VA clinician or third-party provider, the examiner’s job is to evaluate how your condition aligns with the VA’s rating criteria for spinal disabilities.
Medical History and Functional Impact
The examination starts with a detailed review of your medical history. The C&P examiner will ask about your symptoms, flare-ups, treatment history (like physical therapy, injections, or surgeries), and how back pain affects your daily life, including your ability to work, sleep, drive, or handle household tasks.
Make sure to discuss how often flare-ups occur, their duration, and how they limit your mobility. Even if you aren’t experiencing one during the exam, these episodes are considered under VA’s functional loss criteria and can increase your overall disability rating for back pain.
Range of Motion and Physical Examination
During the physical exam, the provider will use a goniometer to measure your range of motion, how far you can bend, twist, or extend. Stop as soon as pain begins, don’t force movement, as this can reduce your disability rating.
They will also observe signs like muscle spasms, guarding, abnormal gait, and signs of nerve involvement, such as radiculopathy or sciatica.
How to Prepare for the C&P Exam
To prepare for the C&P examination, bring relevant medical records, including imaging results and treatment history. Be honest while describing the severity and frequency of symptoms without exaggeration. This ensures a thorough and accurate assessment of your back condition.
Gaining a Favorable VA Rating for Back Pain
With extensive documentation and compelling evidence, you can notably improve both your back pain VA rating and monthly compensation. Here’s how you can support a VA disability claim for back pain by taking the right steps.
1. Keep a Symptom and Flare-Up Log
Start documenting your back pain daily. Include pain levels, triggers (like walking, lifting, or standing), assistive device use, and how the pain limits your activities. If you experience flare-ups, record how long they last and what you’re unable to do during those episodes. This evidence can support a higher VA disability rating based on functional loss.
2. Submit a Nexus Letter
A strong, well-written nexus letter from a qualified physician can medically connect your back condition directly to your military service or link secondary conditions like radiculopathy or depression. While never required, these can sometimes be helpful.
3. Write a Personal Impact Statement
Submit a personal statement as part of your VA disability claim, briefing on how your back condition affects your life. For instance:
- “I cannot sit for more than 30 minutes without shooting pain.”
- “I use a back brace daily and rely on a cane when walking more than 100 feet.”
- “Back spasms force me to lie down for hours several times per week.”
This can help you stay focused during the C&P exam and ensure you mention all relevant symptoms.
4. Gather Lay Statements
Ask your spouse, coworkers, or friends to write short statements explaining how they see your condition affecting you. For example, they can mention if they see you struggle to stand, use a brace, or avoid physical activities you used to enjoy. These buddy statements may reinforce your claim.
5. Provide Outside Medical Evidence
Don’t rely solely on VA treatment notes. Include MRIs, private doctor evaluations, prescriptions, chiropractor reports, and physical therapy records that support the severity of your back condition. If you use a cane, back brace, or TENS unit, include proof of use.
6. Be Detailed During the C&P Exam
Explain exactly how your service-connected condition impacts your life, including work, sleep, mobility, and personal care. Be honest, but don’t minimize your back pain symptoms. Mention flare-ups, assistive devices, and any tasks you can no longer do. Ensure the examiner uses a goniometer to measure your range of motion.
7. Claim All Secondary Conditions as Applicable
Conditions like sciatica, sleep disturbances, mental health issues, or leg numbness often stem from chronic back pain. Effectively claiming these secondary disabilities can significantly increase your combined VA rating. Avoid “pyramiding” as the VA regulations prohibit rating the same symptoms under multiple diagnoses.
Conclusion
Gaining clarity on how the VA rates back pain is the first step toward a successful disability claim and receiving the benefits you have earned. By learning how the VA evaluates spinal conditions, documenting your limitations, and identifying secondary issues, you can present a strong, well-supported claim. Utilize medical evidence, service records, and professional guidance to build your case. With preparation and persistence, veterans can achieve fair compensation and improve their quality of life through the VA disability system.
FAQs
How do I file a back pain VA claim?
To file a VA claim for back pain, submit VA Form 21-526EZ with medical evidence, service records, and a nexus letter linking your condition to military service.
What is the average VA disability rating given for back pain?
On average, VA rating for back pain ranges between 10% and 20%, depending on the veteran’s range of motion and functional limitations.
How can I get 100% VA disability for back pain?
To receive a 100% rating for back pain, a veteran must have unfavorable ankylosis of the entire spine or qualify for TDIU due to an inability to maintain substantially gainful employment.
How does the VA determine back pain?
The VA determines back pain ratings using range of motion measurements, presence of ankylosis, incapacitating episodes for IVDS, and the impact of pain on daily functioning.
What steps to take if my VA disability for back pain is denied?
If your VA disability claim for back pain is denied, you can file a Supplemental Claim with new evidence, request a Higher-Level Review, or appeal to the Board of Veterans’ Appeals.
What additional VA benefits are granted for back conditions?
Veterans with back conditions may receive extra benefits like Special Monthly Compensation (SMC), Aid and Attendance, housing and vehicle grants, clothing allowance, and compensation for assistive devices.
Also read: Nexus Letter for Low Back Pain VA Disability Claim (With Examples)
At Prestige Veteran Medical Consulting, a veteran-owned company, we specialize in Independent Medical Opinions (IMOs) known as Nexus letters.
Our purpose is to empower YOU, the veteran, to take charge of your medical evidence and provide you with valuable educational tools and research to guide you on your journey.
Understanding the unique challenges veterans face, our commitment lies in delivering exceptional service and support.
Leveraging an extensive network of licensed independent medical professionals, all well-versed in the medical professional aspects of the VA claims process, we review the necessary medical evidence to incorporate in our reports related to your VA Disability Claim.
Prestige Veteran Medical Consulting is not a law firm, accredited claims agent, or affiliated with the Veterans Administration or Veterans Services Organizations. However, we are happy to discuss your case with your accredited VA legal professional.



















One Response