Updated: August 23, 2025. Originally published November 2023.
Living with jaw pain, headaches, or constant clicking when you eat may seem like “just part of life,” but for many veterans, these are signs of Temporomandibular Joint Disorder (TMJ). Service often takes a toll on the body through trauma, stress, or grinding brought on by PTSD. The Department of Veterans Affairs recognizes TMJ as a compensable disability, and understanding how it’s rated is the first step to securing the compensation and care you deserve.
This blog explains the VA TMJ rating system, the role of secondary conditions like PTSD and tinnitus, and what evidence veterans need to strengthen their disability claims.

Table of Contents
What Is Temporomandibular Joint Disorder (TMJ/TMD)?
According to the National Institute of Dental and Craniofacial Research, Temporomandibular Joint Disorder (TMJ/TMD) is a condition affecting the jaw joints and chewing muscles, leading to pain, clicking, or limited movement. In veterans, it often develops after head or neck trauma, blast exposure, or stress-related clenching, and may qualify for VA disability when service-connected.
What Happens in a TMJ Disorder?
The temporomandibular joints, located just in front of your ears, connect your lower jaw to the skull and act like sliding hinges for chewing, speaking, and yawning. When the joint, its disc, or the surrounding chewing muscles stop working smoothly, you may develop a temporomandibular disorder (TMD).
Common Symptoms
- Jaw pain, stiffness, or tenderness
- Clicking, popping, or grinding noises during movement
- Trouble chewing or speaking
- Locking of the jaw (open or closed)
- Headaches, neck pain, or ear fullness
- Tinnitus or dizziness
These problems can make everyday tasks like eating and talking difficult, and in severe cases, affect nutrition, sleep, and overall quality of life.
TMJ in Veterans
Research shows that veterans with PTSD experience higher rates of TMJ symptoms, making it a common secondary condition.
For veterans, TMJ often traces back to:
- Trauma or injury from combat or training
- Blast exposure from IEDs or pressure waves
- Chronic stress/PTSD, which increases teeth grinding (bruxism)
- Arthritis or musculoskeletal strain from years of military service
If these service factors caused or aggravated your jaw problems, the VA recognizes TMJ/TMD for compensation under Diagnostic Code (DC) 9905. Disability ratings are based on how wide you can open your mouth (measured in millimeters) and whether you require a modified diet (soft, pureed, or liquid foods).
A systematic review of war veterans found that 56% of those with PTSD experienced temporomandibular disorder (TMD) symptoms, compared with 20% of veterans without war exposure, showing more than double the risk.
How the VA Rates TMJ Disorders
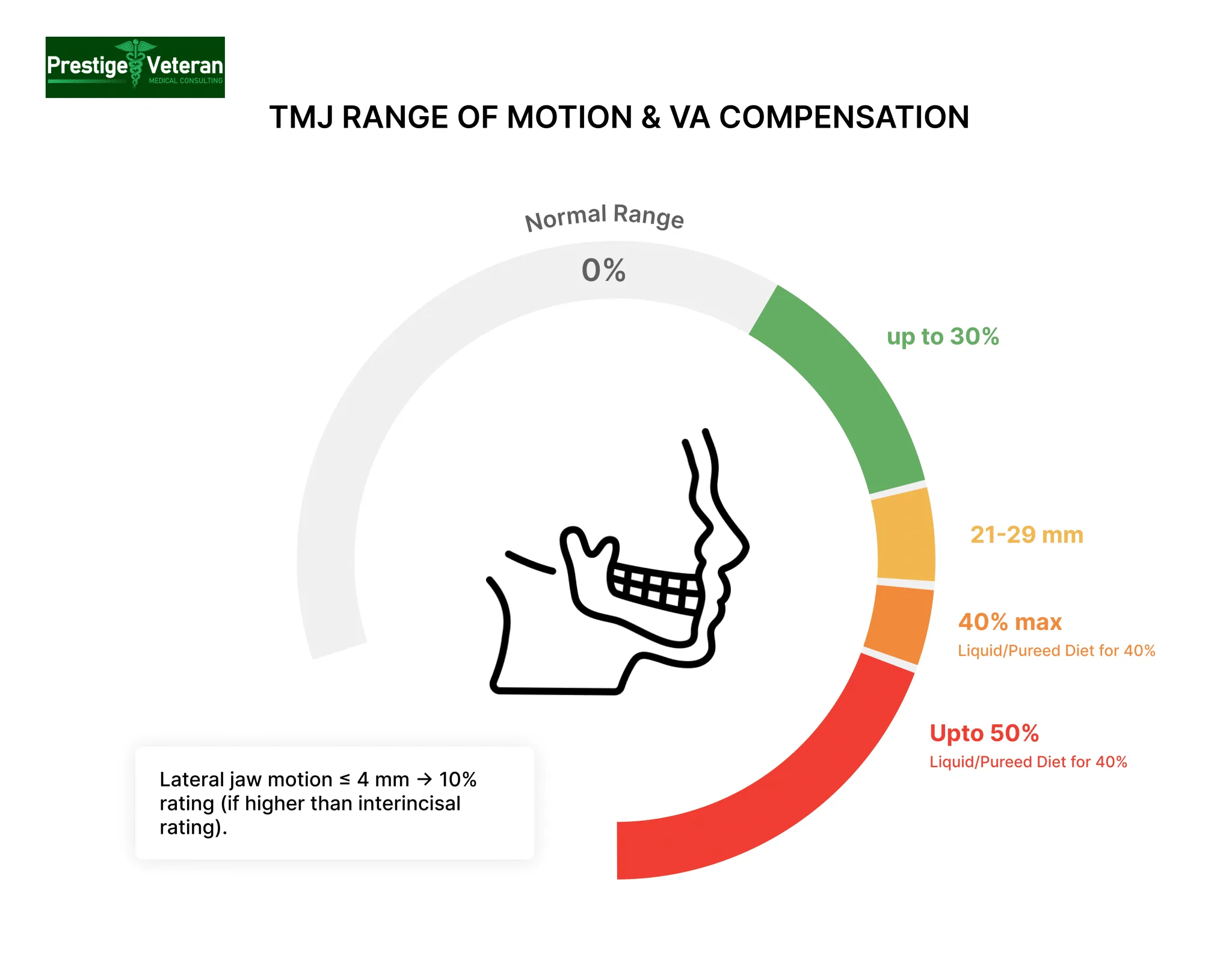
The Department of Veterans Affairs (VA) evaluates Temporomandibular Joint (TMJ) disorders under 38 CFR § 4.150, Diagnostic Code 9905 of the Schedule of Ratings for Dental and Oral Conditions. The VA assigns disability ratings based primarily on three factors:
- Interincisal Range (IR): How wide you can open your mouth (measured in millimeters).
- Lateral Excursion Range: How far you can move your jaw side-to-side.
- Dietary Restrictions – Whether the veteran must rely on “mechanically altered foods,” such as liquids, pureed meals, or soft and semi-solid foods, because of TMJ pain and limited jaw function.
VA Disability Rating for TMJ: Diagnostic Code 9905
The VA disability rating for TMJ under Diagnostic Code 9905 ranges from 10%, 20%, 30%, 40% to 50%, depending on maximum unassisted interincisal opening (mm) and whether a physician has recorded a mechanically altered diet. Higher percentages are assigned for more severe jaw limitations and stricter dietary restrictions.
Here’s the official VA rating schedule for TMJ:
Interincisal Range of Motion (Vertical Opening of the Jaw)
- 0 to 10 millimeters (mm)
- With physician-documented restrictions to all mechanically altered foods → 50% rating
- Without dietary restrictions → 40% rating
- 11 to 20 mm
- With restrictions on all mechanically altered foods → 40% rating
- Without dietary restrictions → 30% rating
- 21 to 29 mm
- With restrictions to full liquid and pureed foods → 40% rating
- With restrictions to soft and semi-solid foods → 30% rating
- Without dietary restrictions → 20% rating
- 30 to 34 mm
- With restrictions to full liquid and pureed foods → 30% rating
- With restrictions to soft and semi-solid foods → 20% rating
- Without dietary restrictions → 10% rating
For VA compensation purposes, the normal maximum unassisted vertical jaw opening is between 35 mm and 50 mm. If a veteran’s maximum unassisted opening is reduced below this range, the VA assigns a disability rating that reflects the severity of functional loss.
Lateral Excursion (Side-to-Side Jaw Movement)
- 0 to 4 mm → 10% rating
Only one direction of motion (either interincisal or lateral excursion) will be rated, whichever gives the higher disability rating.
Note: To qualify for a rating increase based on mechanically altered foods, the VA requires documentation from a treating physician that your condition requires a texture-modified diet. Simply saying that you avoid solid foods does not meet the requirement.
VA Disability Rating for TMJ (Diagnostic Code 9905)
|
Jaw Opening (mm) |
With Physician-Diagnosed Diet Restriction |
Without Diet Restriction |
VA Rating |
|
0–10 mm |
All mechanically altered foods → 50% |
40% |
40–50% |
|
11–20 mm |
All mechanically altered foods → 40% |
30% |
30–40% |
|
21–29 mm |
Pureed/liquid → 40% Soft/semi-solid → 30% |
20% |
20–40% |
|
30–34 mm |
Pureed/liquid → 30% Soft/semi-solid → 20% |
10% |
10–30% |
|
Lateral excursion 0–4 mm |
— |
— |
10% |
Note: Veterans should not attempt to self-measure their jaw opening. A licensed dentist, oral surgeon, or VA examiner must record the measurements for accuracy.
The Painful Motion Rule for TMJ Ratings
Even if your jaw movement does not meet the millimeter thresholds, you may still qualify for a minimum 10% disability rating under VA’s painful motion principle. The VA recognizes that actual painful motion of the jaw when documented by medical records is compensable. For TMJ disorders, examiners should record pain during opening, side movement, or signs such as popping and spasm. This ensures VA acknowledges functional loss due to pain, not just range limits. Learn more about how VA applies this principle in 38 CFR §4.59.
Service Connection for TMJ
To qualify for VA disability benefits for Temporomandibular Joint Disorder (TMJ), veterans must show a valid service connection. This means proving the condition began in service or that another service-connected disability caused or aggravated it. VA recognizes both direct and secondary service connections for TMJ claims.
Direct Service Connection for TMJ
To establish a direct service connection, you must meet three requirements:
- Current Diagnosis – A formal diagnosis of TMJ disorder from a dentist, oral surgeon, or physician, often confirmed with imaging (X-ray, CT, MRI).
- Evidence of an In-Service Event or Injury – Documentation of a jaw injury, facial trauma, blast exposure, or other relevant event during service.
- Nexus (Medical Link) – A doctor’s opinion stating your current TMJ is “at least as likely as not” related to your military service.
Even if TMJ pre-existed service, VA can grant benefits if evidence shows it was aggravated by duty demands.
Example: A veteran injured in a Humvee accident suffers facial trauma. Years later, they develop chronic TMJ. A medical opinion confirms the TMJ is tied to the service-related accident.
The Role of PTSD, Tinnitus, and Other Secondary Conditions
Many veterans establish a secondary service connection for TMJ when an existing service-connected disability causes or worsens TMJ disorder. In these cases, VA compensation is awarded for TMJ as part of the veteran’s overall disability rating.
- PTSD related Bruxism: Veterans with PTSD experience significantly higher rates of TMJ dysfunction. Stress, hyperarousal, and anxiety often lead to bruxism (teeth grinding or clenching), which places constant strain on the jaw joint.
- Tinnitus and TMJ: Because the temporomandibular joint is close to the ear canal, inflammation and misalignment can trigger or aggravate tinnitus (ringing in the ears).
- Neck, Spine, and Musculoskeletal Conditions: Cervical spine injuries or chronic neck pain can alter muscle balance and jaw alignment, creating or worsening TMJ symptoms. TMJ is also reported in veterans with service-connected traumatic brain injuries (TBI) due to muscular and neurological strain.
- Headaches/Migraines: Jaw dysfunction frequently leads to tension headaches and migraines.
- Bruxism: Chronic teeth grinding, often linked to PTSD or anxiety, worsens TMJ. However, VA does not rate bruxism as a separate condition and is usually considered a symptom that may be factored into your TMJ rating or recognized as secondary to another service-connected condition like PTSD.
Filing TMJ as secondary to PTSD or tinnitus can strengthen your claim and potentially increase your overall VA disability rating.
Tip: Always include a medical nexus letter connecting TMJ to your primary service-connected condition. Without this link, the VA may deny your secondary claim.
The Link Between TMJ and PTSD in Veterans
There is a well-documented connection between temporomandibular joint disorder (TMJ) and post-traumatic stress disorder (PTSD), particularly in veterans. PTSD often keeps the body in a constant state of “fight-or-flight,” which activates jaw muscles and leads to clenching or bruxism (teeth grinding). This repetitive strain can inflame the temporomandibular joint, causing symptoms such as chronic jaw pain, headaches, earaches, and limited mouth opening.
Research indicates that veterans with PTSD are up to four times more likely to develop TMD compared to the average military population, underscoring the strong link between psychological trauma and jaw disorders.
For instance, a combat veteran who developed PTSD after exposure to an IED blast may unconsciously grind his teeth at night. Over time, this grinding erodes the cushioning in the joint, resulting in painful TMJ dysfunction that makes chewing and speaking difficult.
For VA disability purposes, TMJ can be rated as a secondary condition to PTSD if medical evidence shows the disorder was caused or aggravated by PTSD. Veterans already service-connected for PTSD can file a secondary claim for TMJ to seek additional compensation.
What to Expect at a C&P Exam for TMJ
A VA Compensation & Pension (C&P) exam for Temporomandibular Joint Disorder (TMJ) is a critical step in the VA disability process. This evaluation helps the VA determine the severity of your condition, how it affects your function, and whether it’s connected to your military service.
What Happens During the TMJ C&P Exam?
The examiner—typically a VA dentist, oral surgeon, or trained medical provider—will perform a physical exam and review your records. During the exam, they will:
- Measure jaw opening (in millimeters)
- Test side-to-side jaw movement
- Observe for locking, clicking, or pain
- Review service and medical records
- Ask about diet (soft/liquid food restrictions)
- Evaluate related conditions like headaches or tinnitus
Bring dental/medical records, imaging, and treatment notes. If you require a special diet, make sure it’s documented in your VA file before the exam. Don’t downplay your symptoms and be specific about pain, flare-ups, and how TMJ limits eating, speaking, or working.
The Role of the DBQ
As part of the evaluation, the examiner may complete a TMJ Disability Benefits Questionnaire (DBQ). This standardized form captures both clinical findings and your reported symptoms that may directly affect your VA rating decision.
Finally, the examiner may also provide a medical nexus opinion linking your TMJ to your military service. Because the C&P exam often influences VA’s decision-making process, thorough preparation can greatly improve your chances of receiving an accurate rating.
TDIU and TMJ: Can Jaw Disorders Qualify You for 100% Pay?
The maximum schedular rating for TMJ (temporomandibular joint disorder) is 50%, which alone usually isn’t enough to qualify for Total Disability based on Individual Unemployability (TDIU). However, TMJ can contribute significantly when combined with other service-connected disabilities like PTSD, migraines, or cervical spine issues. If your overall conditions together make it impossible to maintain substantially gainful employment, you may qualify for TDIU, which pays at the 100% rate.
To meet schedular thresholds under 38 C.F.R. § 4.16:
- You need either one disability rated at 60% or more, or
- A combined rating of 70% with one condition at 40% or higher.
For instance, a veteran with TMJ rated at 40%, along with other service-connected conditions like PTSD rated at 50% and migraines at 30% may qualify for TDIU if these disabilities together prevent working on a full-time job.
Always document your work impact and speak with a VSO or accredited representative to strengthen your TDIU claim.
Evidence That Helps Win TMJ VA Claims
Winning a VA claim for temporomandibular joint disorder (TMJ) depends on submitting strong, detailed, and medically verified evidence. The VA evaluates claims under Diagnostic Code 9905, which focuses heavily on jaw measurements, diet restrictions, and functional loss, so each piece of documentation should be precise and credible.
- Medical diagnosis and measurements – Obtain a current diagnosis from a qualified provider such as a dentist, oral and maxillofacial surgeon, ENT, or physician. Ensure they record the exact interincisal opening (in millimeters) and lateral excursion. These measurements are crucial since VA ratings increase as jaw motion decreases. Ask your clinician to note if a texture-modified diet (soft, pureed, or liquid foods) is medically necessary and specify the duration.
- Imaging and treatment history – X-rays, CT scans, and MRIs strengthen claims by showing structural issues. Document any history of splints, physical therapy, injections, or surgery, as these confirm the seriousness of your condition.
- Lay statements and diaries – First-hand accounts from spouses, coworkers, or supervisors can describe how TMJ flare-ups cause locking, difficulty eating or speaking, and missed work. A two- to four-week symptom diary noting painful foods, jaw locking, and headaches provides contemporaneous proof that examiners value.
- Compensation & Pension (C&P) exam preparation – Expect a VA examiner to review history, measure jaw range of motion, and ask about diet restrictions. Bring your bite splint, recent imaging, specialist notes, and your food diary. Make sure pain on motion is noted, as this can influence ratings under VA’s painful motion rule.
Together, these elements build strong evidence that supports higher, accurate TMJ ratings.
How to File a TMJ VA Disability Claim (Step-by-Step)
Filing a TMJ claim with the Department of Veterans Affairs requires a structured approach to meet evidentiary standards. Following these steps ensures your application is complete and persuasive.
Step 1: File VA Form 21-526EZ. This is the primary application for disability compensation. You can submit it:
- Online through VA.gov
- By mailing the completed form to the VA
- Or seek help from an accredited Veterans Service Officer (VSO).
Download VA Form 21-526EZ from the official forms page.
Step 2: Gather medical evidence. Attach your TMJ diagnosis, precise jaw measurements (in millimeters), imaging results, and physician statements about diet restrictions. Ask your provider to use clear terms such as “mechanically altered foods medically required due to TMJ.”
Step 3: Establish service connection. Provide a nexus letter from a clinician linking TMJ to your service or to another service-connected condition (e.g., PTSD-related bruxism). The standard language, “at least as likely as not” in your nexus letter, is critical for VA acceptance.
Step 4: Prepare for the C&P exam. Bring your food diary, bite splint, and treatment notes. Be honest about flare-ups, locking, and eating difficulties. Examiners will measure jaw motion, and accurate reporting ensures proper rating under DC 9905.
Step 5: Track and respond. Monitor your claim status through VA.gov. If VA requests more evidence (known as a “duty to assist” letter), reply promptly to avoid delays.
Step 6: Appeal if necessary. If your claim is denied or underrated, file a Notice of Disagreement (NOD) within one year. Consider working with an accredited VSO or attorney to improve your chances of securing a favorable VA disability rating for TMJ.
Appeal Options for Your TMJ VA Claim
If your TMJ claim is denied or underrated, you have the following VA decision‑review options:
- Supplemental Claim: Submit new evidence like updated medical records, updated jaw imaging, or a stronger nexus letter.
- Higher-Level Review: Request a more experienced VA reviewer to reevaluate your case.
- Board Appeal: Take your case to the Board of Veterans’ Appeals for a detailed review and decision.
You can also file for an increased rating if your TMJ worsens over time (e.g., loss of jaw mobility, stricter dietary restrictions). Veterans should remember that the VA requires any appeal to be filed within one year of the date on your VA decision letter, or you may lose the right to challenge your TMJ rating.
You can find more details about this in the Board Appeal section of the VA Decision Reviews and Appeals page, explained under the AMA process.
Real-Life Examples of TMJ VA Claims
Veteran Case 1:
A training accident left a veteran with lingering jaw soreness that never fully went away. Over the years, the discomfort progressed into stiffness, clicking, and occasional locking while eating. Imaging confirmed TMJ damage, and a medical opinion connected it to the in-service trauma. This evidence supported direct service connection, qualifying the veteran for VA compensation.
Veteran Case 2:
A veteran living with PTSD noticed severe jaw tension during stressful moments and grinding at night. Over time, this constant clenching caused headaches, ear pain, and trouble opening the mouth. Medical records documented TMJ symptoms, and a private dentist confirmed the condition was aggravated by PTSD. This secondary service connection for TMJ allowed the veteran to receive additional VA benefits.
Veteran Case 3:
During a C&P exam, a veteran’s maximum jaw opening measured just 18 mm, and their doctor confirmed the need for a soft diet because of pain and limited movement. Under VA rating criteria for TMJ, this evidence supported a 40% rating, showing how precise measurements and medical documentation directly shape compensation.
Many veterans find it helpful to get professional assistance from an accredited VSO, claims agent, or VA attorney when navigating a VA claim for TMJ.
VA Dental Care For Service-Connected TMJ
If your Temporomandibular Joint Disorder (TMJ) is service-connected and you receive a VA disability rating of 10% or higher, you may qualify for VA Dental Class I, which provides access to any needed dental care. VA provides comprehensive dental treatment, including exams, jaw therapy, splints, and surgical options if necessary.
Eligibility for VA dental care may require:
- An official TMJ diagnosis
- Medical nexus linking it to the service
- Supporting evidence like X-rays or CT scans
- Veterans with TMJ who must follow a mechanically altered diet, such as soft or pureed foods, should ensure this is documented by a physician, since it can support both a higher disability rating and stronger eligibility for care.
Recently separated veterans may also qualify for one-time dental benefits under Class II if they apply within 180 days of discharge. Additional categories, like former POWs or veterans rated 100%, may also qualify for full dental benefits.
For the most accurate and up-to-date guidance, review the official VA Dental Benefits eligibility page or speak with a VA representative about your jaw disorder.
Conclusion
TMJ may start with jaw pain or clicking, but for veterans, it often reflects the deeper toll of service, stress, trauma, and sacrifice that deserve recognition. By understanding how the VA rates TMJ, preparing strong medical evidence, and linking it to service-connected conditions like PTSD or tinnitus, you can strengthen your claim and secure benefits that make a real difference. Remember: your story, documentation, and persistence carry the most weight. If TMJ affects your daily life, don’t minimize it; your service matters, and so does your right to the care and compensation you’ve earned.
Disclaimer
This article is for general education and does not replace medical care, legal guidance, or representation. Always consult a qualified clinician for diagnosis and treatment, and a VSO or accredited representative for claims strategy.
FAQs
What is the VA disability rating for TMJ?
The VA rates Temporomandibular Joint Disorder (TMJ) under Diagnostic Code 9905 from 10% to 50%, depending on jaw opening (in millimeters) and whether a physician requires a mechanically altered diet.
What is the VA three-finger test for TMJ?
The “three-finger test” is a quick screening to check if you can fit three fingers vertically between your teeth; if not, your interincisal range may fall below the VA’s normal 35–50 mm opening standard. It is a common method to evaluate temporomandibular joint (TMJ) disorders.
Is TMJ considered a VA disability?
Yes, TMJ is a recognized VA disability if service connection is proven through injury, trauma, or a secondary link to another service-connected condition.
Can TMJ be claimed as secondary to PTSD for VA benefits?
Yes, veterans can claim TMJ as secondary to PTSD since stress and bruxism (teeth grinding) linked to PTSD often aggravate jaw disorders.
Can TMJ be rated secondary to tinnitus by the VA?
Yes, TMJ can be filed as secondary to tinnitus because jaw dysfunction near the ear canal can trigger or worsen ringing in the ears.
How does the VA rate bruxism and TMJ together?
The VA does not assign a separate rating for bruxism, but if it causes or worsens TMJ, the condition is rated under Diagnostic Code 9905 from 10% to 50%, potentially increasing overall disability compensation.
Also read: Obstructive Sleep Apnea Secondary to TMJ in Veterans Disability
At Prestige Veteran Medical Consulting, a veteran-owned company, we specialize in Independent Medical Opinions (IMOs) known as Nexus letters.
Our purpose is to empower YOU, the veteran, to take charge of your medical evidence and provide you with valuable educational tools and research to guide you on your journey.
Understanding the unique challenges veterans face, our commitment lies in delivering exceptional service and support.
Leveraging an extensive network of licensed independent medical professionals, all well-versed in the medical professional aspects of the VA claims process, we review the necessary medical evidence to incorporate in our reports related to your VA Disability Claim.
Prestige Veteran Medical Consulting is not a law firm, accredited claims agent, or affiliated with the Veterans Administration or Veterans Services Organizations. However, we are happy to discuss your case with your accredited VA legal professional.


















One Response