In the realm of veteran healthcare, certain injuries can have profound implications beyond the immediate physical trauma. One such injury is the anterior cruciate ligament (ACL) tear, which not only affects mobility and stability but can also lead to long-term disability, impacting veterans’ lives even after their service. Leah Bucholz from Prestige Veteran Medical Consulting explores the connection between ACL tears and veterans’ disability benefits, highlighting the importance of proper care and support.
What is an ACL Tear?
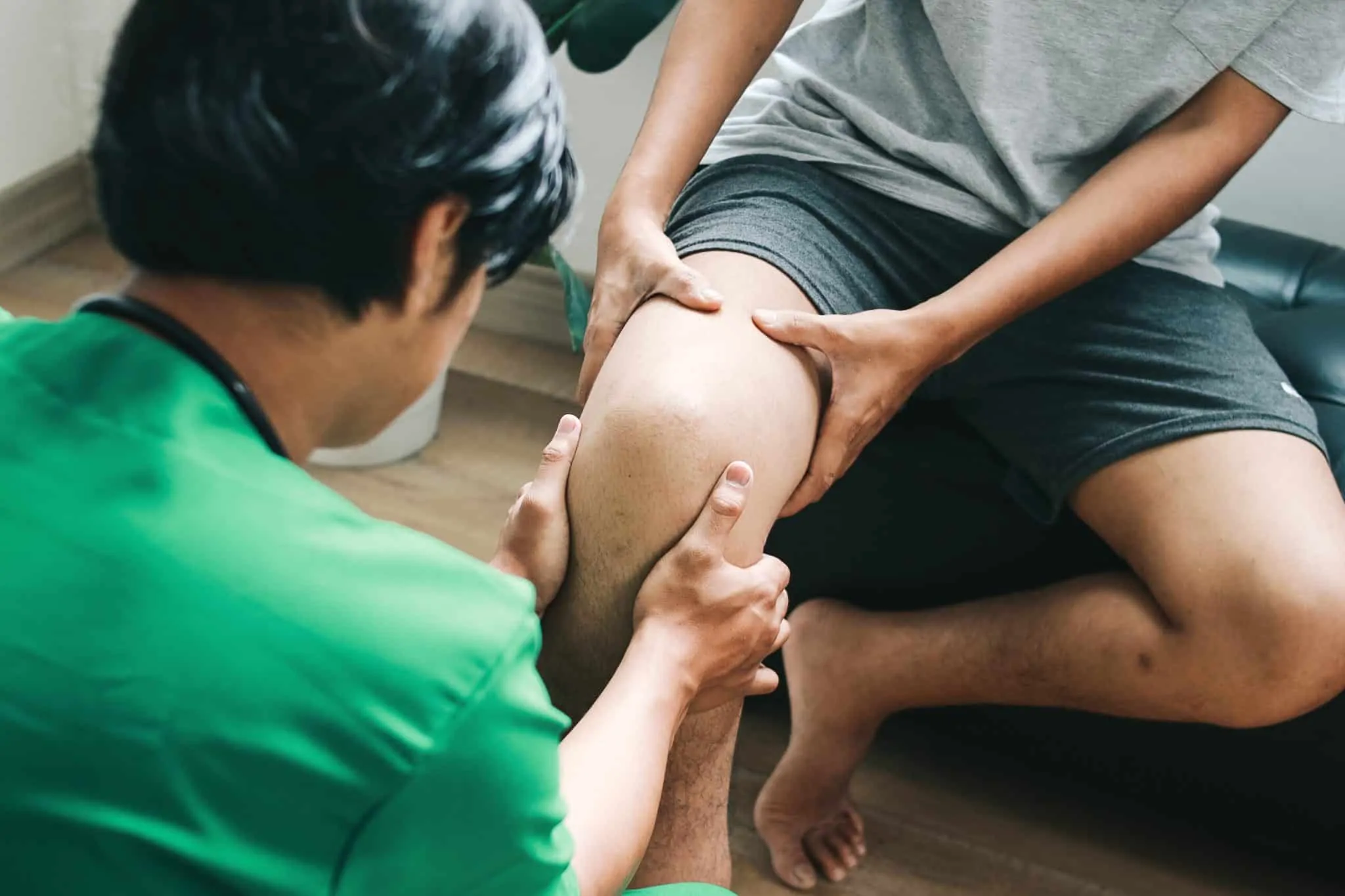
The ACL is one of the major ligaments in the knee joint, crucial for maintaining stability during movement. To comprehend the implications of an ACL tear, it’s essential to grasp the knee’s anatomy. The thigh bone (femur) meets the shinbone (tibia), with the patella (kneecap) and associated ligaments facilitating movement and stability.
An ACL tear can occur due to various factors, including sudden changes in direction, direct impact, or repetitive stress. Military personnel, engaged in physically demanding activities, are particularly susceptible to such knee injuries, whether during training exercises or combat situations.
ACL tear treatments include surgical (like ACL reconstruction surgery) and non-surgical options (such as physical therapy). For veterans, choosing the right treatment depends on individual needs, urgency for recovery, and health conditions. Advanced ACL tear treatments at VA facilities offer specialized care tailored to veterans’ recovery requirements.
Table of Contents
Risk Factors for ACL Tears in Veterans
Military service veterans face unique ACL tear risk factors due to high-impact activities, rugged terrain navigation, and heavy load-carrying. Rigorous training routines, rapid direction changes, and strenuous combat drills increase the likelihood of ACL injuries among veterans. Studies show that anterior cruciate ligament (ACL) injuries in U.S. military personnel occur at a rate 10 times higher than the general population due to the physical demands of military duties. Women, both in military and civilian populations, face a 2-8 times higher risk of ACL injury than men.
Understanding the Impact on Veterans
For veterans, an ACL tear can have multifaceted consequences, both physical and administrative. Establishing a service connection for an ACL tear is essential if the injury occurred during active duty or is related to a service-connected condition. Service connection is essential for VA disability benefits, granting veterans access to financial aid and healthcare needed to manage service-related injuries and maintain their quality of life.
Secondary Conditions Related to ACL Tears
ACL tears can lead to secondary conditions such as osteoarthritis, chronic instability, and gait abnormalities. For veterans, these secondary issues may significantly impact mobility and overall health, contributing to further disability. Osteoarthritis, in particular, is a common long-term consequence of untreated ACL injuries, increasing veterans’ eligibility for additional VA benefits.
Chronic knee instability can also limit physical capabilities, affecting veterans’ quality of life. Understanding and documenting these secondary conditions during the VA claims process is essential to ensure veterans receive the appropriate disability compensation and support for all aspects of their knee-related health issues.
Establishing Service Connection for ACL Tears
Veterans seeking VA disability benefits for ACL tears must establish a direct, secondary, or aggravated service connection. Direct service connection is often straightforward, requiring proof of an ACL injury sustained during military service, such as during training or combat, along with a current diagnosis and medical nexus.
Secondary service connection occurs when the ACL tear is linked to another service-connected condition, like a pre-existing knee injury that led to further damage. This requires medical evidence to show how the initial condition contributed to the secondary condition like ACL tear.
Service-connected aggravation applies if an ACL condition existed before service and was worsened by military duties. Veterans must prove the condition deteriorated beyond natural progression due to active duty. The VA assesses how much the condition has changed to determine benefits.
Establishing any of these service connections with detailed evidence is essential for receiving appropriate VA disability compensation for ACL injuries.
Diagnostic Challenges and Complications
Diagnosing an ACL tear typically involves a thorough clinical evaluation combined with diagnostic imaging techniques. X-rays are often used to rule out fractures but can’t detect ligament or tendon damage. Magnetic resonance imaging (MRI) is the preferred method for assessing the severity of an ACL injury and identifying any associated tissue damage, such as cartilage or tendons. Ultrasound may also be used to visualize injuries in the knee’s ligaments, tendons, and muscles. However, complications can arise, particularly if the injury remains untreated or undiagnosed. Chronic ACL tears can lead to associated issues like meniscal tears, exacerbating pain and instability.
Long-Term Implications and Disability
Untreated ACL tears can significantly impact an individual’s quality of life, leading to chronic knee pain, limited mobility, and decreased functional capacity. According to a study report, even with successful surgical knee stabilization, 4% to 35% of individuals with ACL injuries will develop arthrofibrosis, more than half will not regain full active duty status, and up to 50% are likely to develop post-traumatic osteoarthritis (PTOA) within 15 years. Veterans grappling with these challenges may find themselves unable to perform daily activities or pursue gainful employment, necessitating VA disability benefits to support their needs.
Navigating the VA Disability Process
When applying for VA disability benefits for an ACL tear it may be beneficial to have a thorough understanding of the VA’s evaluation process and criteria for disability ratings. Veterans often provide comprehensive medical documentation, showing diagnosis, treatment, or symptoms of ACL tears, including MRI/CT scan results, surgery records, physician’s notes, and evidence of functional limitations. Proof of injury during service or aggravation by service, supported by service treatment records, is also required for disability benefits claims. Collaborating with healthcare providers, including primary care physicians and orthopedic specialists can be crucial in obtaining the necessary documentation and support for the VA disability claim.
VA Ratings for Common Knee Conditions
The VA evaluates knee conditions based on severity, range of motion limitations, muscular injuries, and overall impact on daily life, using specific diagnostic codes to determine appropriate compensation. These ratings are critical for veterans with knee issues, such as ACL tears, arthritis, meniscus injuries, and conditions involving flexion and extension limitations.
For ACL (anterior cruciate ligament) tears, the VA rates under Diagnostic Code 5257, which addresses knee instability. ACL tear VA rating ranges from 10% to 30%, depending on whether the ligament tear leads to persistent instability and whether assistive devices are necessary. A complete ligament tear causing severe instability, requiring a brace and assistive device, may qualify for a 30% VA disability rating, while less severe cases may receive lower ratings.
For knee flexion limitations, rated under Diagnostic Code 5260, the VA assigns ratings from 0% (if flexion is limited to 60 degrees) to 30% (if flexion is limited to 15 degrees).
Extension limitations, rated under Diagnostic Code 5261, are rated between 0% (extension limited to 5 degrees) and 50% (extension limited to 45 degrees), based on how much the knee can straighten.
Muscular injuries impacting the flexion or extension of the knee are rated as slight, moderate, moderately severe, or severe, and can receive ratings of 0%, 10%, 20%, 30%, or 40%, depending on the degree of impairment and loss of function.
Arthritis in the knee is also a common condition evaluated by the VA, generally receiving ratings of 20%, 40%, or 60%, depending on the extent of the degeneration and its impact on mobility. In extreme cases, a veteran with a knee condition may be eligible for a 100% rating, especially if arthritis severely limits daily activities.
Meniscus injuries, often resulting in pain, locking, or fluid on the knee (effusion), are rated under Diagnostic Code 5258 or 5259. If the meniscus tear causes frequent episodes of pain and effusion, a veteran may qualify for a 20% VA disability rating.
For surgical knee repair or replacement, the VA may assign a temporary 100% disability rating during the recovery period, which lasts up to four months post the knee replacement surgery. After this recovery phase, the VA rating for knee pain is re-evaluated to reflect any lasting impairment.
The VA applies a bilateral factor for veterans with disabilities in both knees, adding an additional value to the combined rating. This reflects veterans’ increased difficulty when both legs are affected, ensuring proper VA compensation for the compounded impact on mobility and quality of life.
Addressing the Kinetic Chain Theory
The interconnected nature of musculoskeletal injuries, as described by the kinetic chain theory, underscores the importance of holistic treatment approaches. An ACL tear affects the stability of the entire lower extremity, altering the natural biomechanics of the knee and influencing the movement patterns of both proximal (hip) and distal (ankle, foot) joints. These disruptions often lead to compensatory changes in gait and posture, which can create a cascade of secondary issues, such as hip strain, lower back pain, and ankle problems.
Introduced by Franz Reuleaux and later refined by Dr. Arthur Steindler, the kinetic chain theory highlights how body segments work together for coordinated movement. In ACL rehabilitation, focusing on both open kinetic chain (OKC) and closed kinetic chain (CKC) exercises ensures comprehensive recovery by retraining joint and muscle coordination. This approach reduces the risk of further injury and enhances overall functional recovery. It’s particularly essential for individuals like veterans, who often require a high level of physical resilience and activity.
Conclusion
In conclusion, ACL tears represent more than just a physical injury for veterans—they embody a complex intersection of healthcare, disability, and rehabilitation. By understanding the nuances of ACL tears and their implications for veterans can better advocate for comprehensive care and support within the VA system. Through proactive collaboration between veterans, healthcare providers, and VA representatives, we can ensure that those affected by ACL tears receive the resources and assistance they need to lead fulfilling lives post-service.
Also read: Camp Lejeune water contamination and VA Disability
At Prestige Veteran Medical Consulting, a veteran-owned company, we specialize in Independent Medical Opinions (IMOs) known as Nexus letters.
Our purpose is to empower YOU, the veteran, to take charge of your medical evidence and provide you with valuable educational tools and research to guide you on your journey.
Understanding the unique challenges veterans face, our commitment lies in delivering exceptional service and support.
Leveraging an extensive network of licensed independent medical professionals, all well-versed in the medical professional aspects of the VA claims process, we review the necessary medical evidence to incorporate in our reports related to your VA Disability Claim.
Prestige Veteran Medical Consulting is not a law firm, accredited claims agent, or affiliated with the Veterans Administration or Veterans Services Organizations. However, we are happy to discuss your case with your accredited VA legal professional.